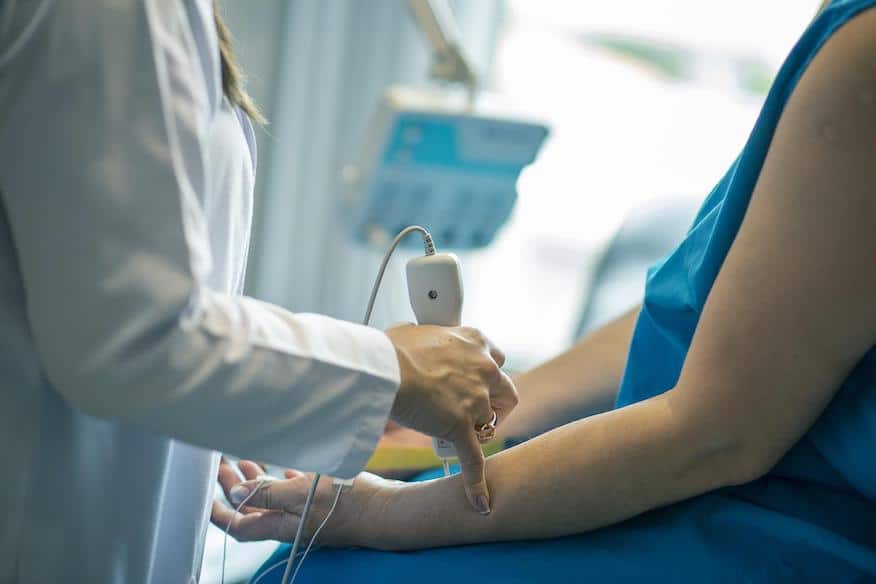
Workers may delay medical treatment because they need prior authorization from the Ohio Bureau of Workers’ Compensation (BWC). However, timely treatment is essential for a full recovery and return to work.
Fortunately, some of these treatments fall under presumptive approval. This means the physicians have presumed approval to provide treatment within the first 60 days following an injury, provided specific criteria are met.
Here are the medical services requiring preauthorization and their exceptions:
- Hospital services: Inpatient and outpatient care in hospitals requires preauthorization unless it is an emergency. All emergency care receives presumptive approval, including diagnostic tests and bone setting.
- Physical medicine services: Chiropractic, osteopathic, manipulative treatment, and acupuncture require pre-approval. However, you can receive up to 12 physical medicine visits before approval, including chiropractic, physical therapy, occupational therapy, and specialized massage therapy.
- Mental health treatment: You need preauthorization if you face mental health conditions due to your injury or a traumatizing event at work. Otherwise, Ohio workers’ compensation insurance will not cover psychological treatment and medication.
- In-home physician services: Workers’ compensation covers the first visit by an in-home nurse or physician. After that, you need preauthorization to ensure future visits receive coverage.
- Dental, vision, and hearing services: All dental work must be preapproved for coverage. Vision and hearing services receive presumptive approval up to $100, and any expenses after that require preauthorization.
- Durable medical equipment: You receive presumptive authorization for walkers, wheelchairs, oxygen tanks, and other equipment up to $250. Purchases and rentals exceeding $250 must obtain preauthorization.
- Non-emergency medical transport: You do not need preapproval of emergency ambulance services. However, scheduled medical transportation must receive preauthorization.
- Diagnostic testing: Unless it is an emergency, exploratory surgery requires preapproval. However, x-rays, MRIs, and CAT scans do not require prior authorization.
- Injections: You can receive up to three soft tissue or joint infections and three trigger point injections without preauthorization. These injections include corticosteroids, anti-inflammatories, and pain relievers. After these first three, you must receive preauthorization.
It takes effort to secure preauthorization. There are several forms to file, and even after those steps, preauthorization is never guaranteed. Workers may find needed treatment is not approved. They may also end up with out-of-pocket costs because they continued treatment, expecting it to be approved.
Workers’ compensation procedures in Ohio are complex and often daunting. If you face challenges receiving coverage for medical bills and lost wages, the attorneys at Dworken & Bernstein are here to help. We offer extensive experience getting workers their needed benefits. Contact us today to schedule a consultation.